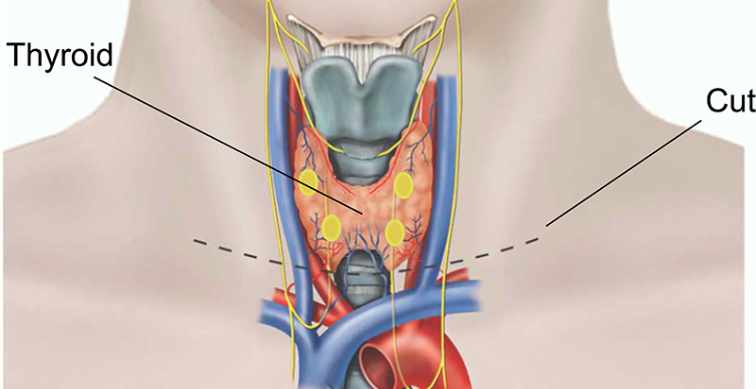
Thyroidectomy
A thyroidectomy is a surgical procedure to remove all or part of the thyroid gland, a butterfly-shaped organ located at the base of the neck that produces hormones that regulate metabolism. Thyroidectomy is typically performed to treat thyroid conditions, such as thyroid cancer, goiter (enlarged thyroid), hyperthyroidism (overactive thyroid), or benign thyroid nodules.
Indications for Thyroidectomy
- Thyroid Cancer: Surgical removal of the thyroid is often necessary for cancer treatment, especially if the cancer is localized and has not spread beyond the thyroid gland.
- Goiter: An enlarged thyroid gland (goiter) that causes symptoms like difficulty swallowing or breathing may require removal if the goiter is large or causes compression of nearby structures.
- Hyperthyroidism: If hyperthyroidism (overactive thyroid) is not controlled by medications or radioactive iodine therapy, thyroidectomy may be necessary to remove the overactive tissue.
- Benign Thyroid Nodules: Large or symptomatic non-cancerous thyroid nodules may require surgical removal if they cause problems such as pain, difficulty swallowing, or breathing issues.
- Thyroid Dysfunction: In some cases, thyroidectomy may be recommended for individuals who have thyroid disease that does not respond to other treatments.
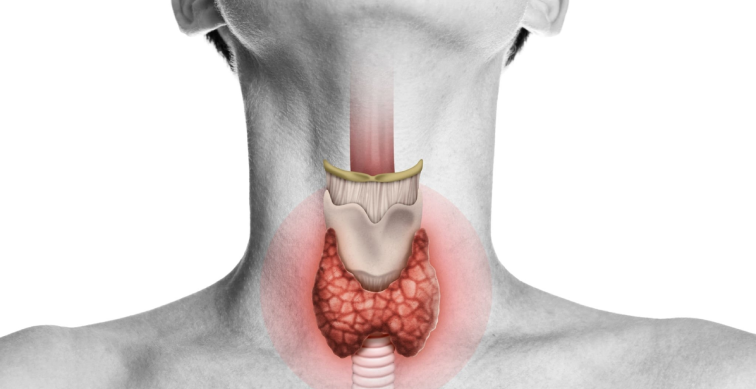
Types of Thyroidectomy
Total Thyroidectomy: This procedure involves the complete removal of the thyroid gland. It is commonly performed for thyroid cancer or if the entire gland is affected by disease.
Partial or Hemithyroidectomy: This involves the removal of only one lobe of the thyroid, typically performed if the thyroid problem is confined to one side of the gland (e.g., a benign nodule or small tumor).
Subtotal Thyroidectomy: This procedure involves the removal of most of the thyroid gland but leaves a small portion of it intact to maintain some thyroid function.
Lobectomy: In cases where there is a single nodule or benign condition affecting one lobe of the thyroid, the surgeon may remove only the affected lobe and leave the other lobe in place.
A thyroidectomy is a highly effective procedure for treating thyroid conditions, including cancer, goiter, and hyperthyroidism. While most people recover well and experience positive outcomes, it is important to carefully follow post-surgical instructions and attend follow-up appointments to monitor thyroid function. Thyroid hormone replacement therapy is essential for individuals who have had a total thyroidectomy, and most patients can lead normal, healthy lives with appropriate treatment.
Complications of Thyroidectomy
- Injury to Nerves: The thyroid is located near important nerves, including the recurrent laryngeal nerve, which controls the vocal cords. Damage to this nerve can result in hoarseness, difficulty speaking, or swallowing problems.
- Hypocalcemia: The parathyroid glands, which regulate calcium levels, are located near the thyroid. If the parathyroid glands are damaged or removed during surgery, it can lead to low calcium levels (hypocalcemia), resulting in symptoms such as muscle cramps, tingling, or numbness.
- Infection: As with any surgery, there is a risk of infection at the incision site.
Prevention and Management
- Iodine: Ensure adequate iodine intake, as iodine is essential for thyroid function. Deficiency can lead to goiter or hypothyroidism. Iodized salt is a common source of iodine.
- Regular Check-Ups: Regular thyroid screenings, especially for individuals with a family history of thyroid disease, can help detect conditions early and prevent complications.
- Healthy Diet: A balanced diet rich in vitamins and minerals supports overall thyroid health.
