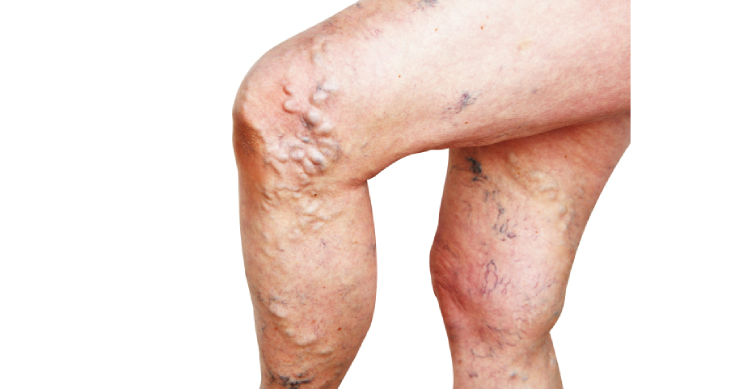
Varicose Veins
Varicose veins are enlarged, twisted veins that often appear on the legs and feet. They occur when the valves inside the veins that help blood flow back to the heart become weakened or damaged, causing blood to pool in the veins. This leads to the veins becoming swollen, stretched, and visibly prominent under the skin. Although they are typically not dangerous, varicose veins can cause discomfort and, in some cases, more serious health issues.
Symptoms
- Visible Swollen Veins: The most obvious sign is the appearance of dark purple or blue, bulging veins under the skin, often on the legs and feet.
- Pain or Discomfort: Some people experience aching, heaviness, or throbbing in the legs, especially after prolonged standing or sitting.
- Swelling: Swelling of the lower legs, especially after standing for long periods.
- Itching or Burning Sensation: The skin around varicose veins may itch or feel irritated.
- Cramps: Muscle cramps, especially at night, can occur in the lower legs.
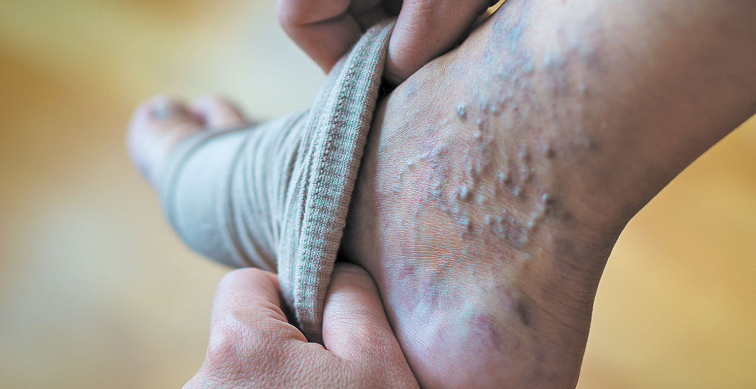
- Skin Changes: Over time, the skin around varicose veins may become discolored, dry, or develop ulcers
Treatment Options
Conservative Measures
- Compression Stockings: These stockings apply pressure to the legs and help improve circulation, reducing pain and swelling.
- Exercise: Regular physical activity, particularly walking, helps improve circulation and can reduce symptoms.
- Leg Elevation: Elevating the legs when sitting or lying down can help reduce swelling and alleviate discomfort.
Medical Procedures
- Sclerotherapy: A solution is injected into the varicose veins, causing them to shrink and eventually fade away. This is often used for smaller veins.
- Laser Treatment: Laser therapy can be used to close off varicose veins by applying concentrated light to the vein walls, causing them to collapse and seal shut.
- Endovenous Laser Therapy (EVLT): This procedure uses laser energy to treat larger varicose veins by heating the vein from the inside, causing it to collapse.
- Radiofrequency Ablation (RFA): Similar to EVLT, RFA uses heat from radiofrequency energy to close off the affected veins.
Self-Care
- Avoid Prolonged Standing or Sitting: Change positions regularly to reduce pressure on the veins.
- Wear Compression Garments: Special stockings help improve circulation in the legs.
- Elevate the Legs: Elevating the legs above heart level can help reduce swelling and improve circulation.
Varicose veins are common and often treatable with lifestyle changes, medical interventions, and self-care strategies. If symptoms become bothersome or if complications arise, it’s important to consult with a healthcare provider for an appropriate treatment plan.
Causes and Risk Factors
- Aging: As people age, the veins lose elasticity and the valves weaken, increasing the risk of varicose veins.
- Genetics: A family history of varicose veins increases the likelihood of developing them.
- Gender: Women are more likely to develop varicose veins, likely due to hormonal changes during pregnancy, menstruation, or menopause. Hormones can relax the vein walls, making them more prone to dilation.
- Pregnancy: The increased blood volume during pregnancy and the pressure of the growing uterus on the veins can contribute to the development of varicose veins.
Prevention and Management
- Exercise Regularly: Staying active improves circulation and helps prevent blood from pooling in the veins.
- Maintain a Healthy Weight: Reducing excess weight reduces pressure on the veins.
- Avoid Prolonged Sitting or Standing: Take regular breaks if your job or daily routine involves standing or sitting for long periods.
- Wear Compression Stockings: If you are at risk for varicose veins or already have them, compression stockings can help prevent worsening symptoms.
